Claims Management Software For Faster Claim Resolution: 8 Popular Solutions Reviewed
Claims processes can be quite a hassle with information coming in from different channels, documentation being left incomplete, and coordination taking time. Even a small gap in intake or review can slow resolution and increase operational risk.
Structured claims management software helps bring order to that environment. Instead of relying on scattered emails or spreadsheets, teams can standardize FNOL capture, route cases through defined approval paths, and maintain a clear audit record of every decision.
In this article, we review eight widely adopted claims management software solutions used by insurers and claims operations teams. The focus is on how well each platform supports day-to-day execution, from intake and coverage validation to fraud monitoring, system integrations, and regulatory oversight.
The 8 Claims Management Software (Reviewed In No Particular Order)
Below is a quick overview of the eight widely adopted claims management software solutions for modern insurers.
We didn’t rank tools based on brand recognition. Instead, we examined analyst research and verified feedback from claims professionals on review sites such as G2.
Next, we looked at how each solution (including our own tool, FlowForma) from our compiled list supports important aspects of claims management, including:
- FNOL and structured claims intake
- Coverage checks and risk scoring
- Adjuster review workflows with multi-level approvals
- Evidence capture with traceable audit trails
- Fraud detection and supervisory oversight
- Integrations with policy systems, claims platforms, ERP, or ITSM tools
We additionally considered each platform’s approach to risk and regulatory compliance. We found out that some platforms offer purpose-built insurance functionality, while others rely on configurable workflows to maintain oversight.
P.S. This is not a ranking list. We have simply reviewed the popular claims management software based on real-life use cases and reviews.
|
Claims management tool
|
Best for
|
Key strength
|
G2 rating
|
|
Pipefy
|
Tracking structured claims visually
|
Lets teams follow claims through clear visual pipelines
|
4.6/5
(with 234 reviews)
|
|
Appian
|
Managing complex, extended claims
|
Centralizes claims data with structured case management across teams
|
4.5/5
(with 487 reviews)
|
|
FlowForma
|
Automating approval-heavy claims
|
Enables audit-ready claims workflows with AI assistance on Microsoft 365
|
4.5/5
(97 reviews)
|
|
Guidewire ClaimCenter
|
Modernizing core P&C claims
|
Provides a structured core system for end-to-end claims management
|
4.5/5
(with 41 reviews)
|
|
Nintex
|
Coordinating cross-department claims
|
Orchestrates claims processes with automation and document handling
|
4.3/5
(with 1319 reviews)
|
|
Kissflow
|
Organizing multi-step claims processes
|
Simplifies intake, routing, and approval tracking for claims
|
4.3/5
(with 591 reviews)
|
|
ProcessMaker
|
Automating data-heavy claims
|
Extracts and processes claims data with AI to reduce manual work
|
4.3/5
(with 305 reviews)
|
|
BriteClaims (BriteCore)
|
Integrated claims and policy operations
|
Keeps claims, policy, and billing data unified for fast decisions
|
4.3/5 (with 24 reviews)
|
The 8 popular claims management software
1. Guidewire ClaimCenter
Best for: End-to-end P&C core claims systems
Guidewire’s homepage
Guidewire ClaimCenter is typically used by carriers that are replacing legacy claims platforms and moving to a modern core system. It delivers comprehensive, insurance-specific functionality with deep configuration options and close alignment to policy and billing modules within the Guidewire ecosystem.
The platform is best suited to insurers undertaking full core transformation, particularly those managing high claim volumes and complex P&C operations, rather than teams seeking lightweight workflow automation layered onto existing systems.
Key features of Guidewire ClaimCenter
End-to-end core claims management
ClaimCenter supports the full claims lifecycle, from FNOL and coverage verification through investigation, reserving, payments, recoveries, and closure, all within a single core environment.
Prebuilt insurance data model and workflows
The platform includes a structured data model and predefined claims processes tailored to P&C carriers, which reduces the need to design core claims logic from the ground up.
Configurable business rules and validations
Carriers can configure coverage rules, approval thresholds, and compliance checks to ensure consistent claim handling aligned with policy terms and regulatory requirements.
Integrated reserve and payment management
Built-in financial controls allow claims teams to manage reserves, issue payments, and maintain financial accuracy throughout the lifecycle of each claim.
Guidewire User Ratings on G2
|
Category
|
Guidewire ClaimCenter Rating
|
|
Overall
|
4.5 on G2
|
|
Meets Requirements
|
8.9
|
|
Ease of Use
|
8.6
|
|
Ease of Setup
|
7.4
|
|
Ease of Admin
|
8.7
|
|
Quality of Support
|
8.8
|
|
Has Been a Good Partner in Doing Business
|
9.1
|
|
Product Direction (% positive)
|
9.7
|
Guidewire’s user ratings on G2
Guidewire’s Pros and Cons
Pros:
- Highly customizable for complex, enterprise-scale insurance claims workflows.

Source
- Strong core platform purpose-built for P&C claims management.

Source
- Improves adjuster productivity with structured, end-to-end claim handling.
- Scalable architecture supporting large insurers and high claim volumes.
Cons
- Complex customization requires specialized Guidewire development expertise.

Source
- Upgrades become time-consuming due to heavy prior customizations.
- High implementation and maintenance costs for smaller insurers.
Best for: Approval-heavy, compliance-focused claims automation
FlowForma playground for insurance
If you’re constantly working with approval-heavy claims processes where visibility and regulatory compliance are mandatory, FlowForma is your go-to platform.
Built for regulated insurance environments, FlowForma is an AI-powered, no-code platform that runs natively on Microsoft 365 and supports structured, audit-ready claims management without requiring custom-built applications. It is well-suited to insurers that need tighter control over approvals, documentation, and compliance while maintaining operational speed.
Claims workflows and data, including governance, are aligned with your existing Microsoft security and access controls, which makes rollout and oversight simpler for IT.
Key features of FlowForma
AI Copilot for claims workflow creation
You can describe your claims journey, from FNOL to settlement, in plain language, and AI Copilot will generate structured steps, forms, and routing logic. It accelerates design while keeping workflows consistent across teams.
In this insurance claims automation demo, you’ll see how digital forms adapt instantly to inputs, saving customers and internal teams time.
No-code claims automation
Multi-level approvals, fraud reviews, reserve checks, escalations, and conditional paths can be configured without development work, allowing operations teams to refine processes while IT maintains governance.
Microsoft 365–native claims data
Claims data remains in SharePoint, and tasks surface in Teams and Outlook, so security and permissions continue to follow your existing Microsoft model.
End-to-end audit trails
Every action, approval, and document update is automatically time-stamped and traceable, supporting ongoing regulatory compliance.
Claims performance analytics
Dashboards provide visibility into turnaround times, bottlenecks, and workload distribution, helping you continuously improve claims efficiency.
FlowForma User Rating on G2
|
Category
|
FlowForma Rating
|
|
Overall
|
4.5 on G2
|
|
Meets Requirements
|
8.6
|
|
Ease of Setup
|
8.3
|
|
Ease of Use
|
8.7
|
|
Ease of Admin
|
8.2
|
|
Quality of Support
|
9.2
|
|
No-Code Development Platforms
|
8.6
|
FlowForma’s user ratings on G2
FlowForma's Pros and Cons
Pros:
- Quick and responsive support team
Source
- Delivers smooth workflow automation that accelerates approvals and routine processes
Source
- Enables business users to design and modify workflows without heavy reliance on IT
- Improves coordination and visibility across departments and shared operations

Source
- Drives measurable productivity gains in high-volume, regulated environments

Source
Cons:
- Effective use requires structured process design and a thoughtful, well-planned setup.

Source
- The learning curve can feel steep, especially without structured onboarding and training.

Source
- Navigation takes time to get used to for new or occasional users.

Source
FlowForma's Pricing
FlowForma uses a clear, process-based pricing model. Instead of charging per user or locking features behind higher tiers, pricing is based on the number of workflows you run.
As more teams adopt the platform, departments expand usage, or external stakeholders participate in processes, your costs remain predictable and unchanged.
3. BriteClaims (BriteCore)
Best for: Integrated policy, billing, and claims management

BriteCore homepage
A cloud-based platform, BriteCore helps insurers handle claims efficiently by keeping policy, billing, and claims in one system. It is designed for carriers that need to manage FNOL, investigations, reserves, and payments smoothly, without juggling multiple tools or relying on manual handoffs.
With everything connected, your adjusters can focus on resolving claims quickly and accurately.
Key features of BriteCore
Integrated claims management
From FNOL to payout, all claim activities happen within the same system as policies and billing. Adjusters can move cases through investigation, reserve tracking, approvals, and closure without switching platforms, reducing delays and errors.
Unified data access
Claims teams can instantly access policy details and billing history while reviewing a claim.
Flexible workflows and rules
You can configure approval thresholds, validation checks, and escalation paths to match your underwriting rules and compliance requirements, keeping claims moving smoothly and consistently.
API-driven connectivity
BriteCore integrates with payment providers, document management tools, and external data sources, enabling your team to automate tasks and extend claims capabilities as needed.
BriteCore’s User Ratings on G2
|
Category
|
BriteCore Rating
|
|
Overall
|
4.3 on G2
|
|
Meets Requirements
|
8.7
|
|
Ease of Use
|
9.2
|
|
Ease of Setup
|
8.2
|
|
Ease of Admin
|
9.0
|
|
Quality of Support
|
8.6
|
|
Has Been a Good Partner in Doing Business
|
9.7
|
|
Product Direction (% positive)
|
9.4
|
BriteCore’s user ratings on G2
BriteCore’s Pros and Cons
Pros:
- User-friendly interface simplifies navigation for agents and operations teams.
Source
- Fast onboarding improves adoption across underwriting and policy administration.
- Strong integrations with partner vendors and insurance ecosystem tools.

Source
- Efficient policy management streamlines core insurance operations.
Source
Cons:
- Reporting and analytics capabilities need deeper customization and flexibility.

Source
- Customer support response times vary for non-critical requests.
- Advanced reporting often requires additional configuration or external tools.
4. Appian
Best for: Complex, multi-system claims orchestration
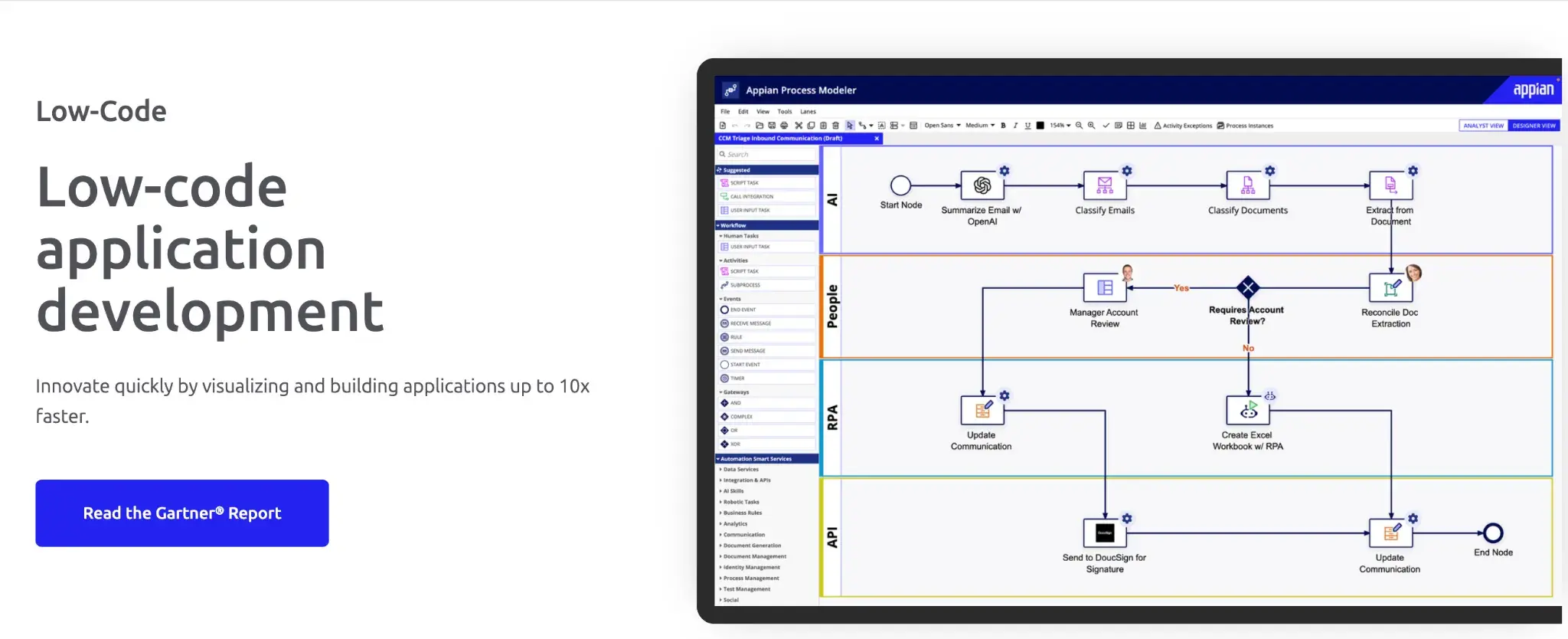
Appian’s low-code development platform
Large insurers managing long-running claims that span multiple systems and teams often rely on Appian. It provides structured case management, enterprise-grade governance, and integration across policy, billing, fraud, and finance systems, enabling organizations to centralize claims data and workflows.
Key features of Appian
Unified claims data with data fabric
Appian’s data fabric connects policy systems, claims platforms, document repositories, and third-party sources into a single layer. Teams can access all relevant claim information without duplicating or migrating data.
Structured process modeling
The platform uses BPMN standards to map claims workflows, including approvals, regulatory checks, and escalation paths, in a standardized, auditable format.
AI for document handling and insights
Built-in AI classifies incoming claims documents, extracts key data from unstructured files, and provides insights to support decision-making.
Case management for extended claims
Appian manages claims involving multiple stakeholders over extended timelines, providing structured oversight through the investigation, review, approval, and settlement stages.
Appian User Ratings on G2
|
Category
|
Appian Rating
|
|
Overall
|
4.5 on G2
|
|
Meets Requirements
|
8.5
|
|
Ease of Use
|
8.7
|
|
Ease of Setup
|
8.5
|
|
Ease of Admin
|
8.5
|
|
Quality of Support
|
8.5
|
|
Has Been a Good Partner in Doing Business
|
8.8
|
|
Product Direction (% positive)
|
9.0
|
Caption: Appian’s user ratings on G2
Pros and Cons of Appian
Pros
- Low-code drag-and-drop interface accelerates rapid application development.

Source
- Intelligent automation improves onboarding and compliance workflows.

Source
- Strong plugin ecosystem supporting enterprise-grade integrations.

Source
- Built-in AI enhances efficiency and reduces manual effort.
Cons
- Expensive licensing model, especially for growing user bases.

Source
- Limited customization for highly complex use cases.

Source
- Steep learning curve for advanced configurations and features.
5. Kissflow
Best for: Structuring multi-step claims or approvals
Kissflow homepage
For teams looking to bring structure to claims that are often handled through email and spreadsheets, Kissflow can be a good solution. While it’s not a dedicated claims platform, it lets your team track each claim through a clear, organized process from intake to resolution, keeping work visible and on track.
Key features of Kissflow
Claims intake and review workflows
Online forms capture claim details and supporting documents, and each submission moves automatically through predefined stages, routing to the appropriate team members at the right time.
Centralized tracking
All claim data, notes, and approval history are stored in a single system. Your team can see the current status in real time, eliminating the need to chase updates across multiple channels.
Claims monitoring apps
Internal apps track claim decisions, reserve amounts, and payment status, with updates happening automatically as the workflow progresses.
Role-based access controls
Permissions determine who can view, update, or authorize each step, keeping sensitive information secure while maintaining accountability throughout the claims process.
Kissflow User Ratings on G2
|
Evaluation Area
|
Kissflow Score
|
|
G2 Aggregate Rating
|
4.3 on G2
|
|
Alignment With Business Needs
|
8.6
|
|
User Friendliness
|
8.8
|
|
Implementation Simplicity
|
8.3
|
|
Administration Experience
|
8.5
|
|
Support Experience
|
8.7
|
|
Partnership Satisfaction
|
8.6
|
|
Roadmap Confidence (% Positive)
|
8.7
|
Kissflow’s user ratings on G2
Kissflow’s Pros and Cons
Pros:
- It is very easy for business users to automate processes quickly.

Source
- Strong cross-department workflow collaboration and visibility.
Source
- Fast digitalization with a simple, guided process setup.
- Flexible customization for adapting workflows to business needs.

source
Cons:
- Reporting and mobile functionality lack advanced capabilities.

Source
- Integration challenges with external enterprise systems.
Source
- Access control setup can feel inconsistent and restrictive.
Source
6. Nintex
Best for: Multi-department workflow coordination
Nintex homepage
For organizations that need to coordinate multi-step processes across departments, Nintex is a reliable tool. It supports the full claims lifecycle, including intake, compliance reporting, and system updates, ensuring that every step is visible and connected.
Key features of Nintex
Workflow orchestration engine
Claims move through each stage with full visibility, allowing teams to act immediately when approvals are pending or bottlenecks arise.
Document generation and eSignature
Letters, forms, and other claim documents are automatically populated from data, with signature routing to speed approvals and reduce manual handling.
RPA for legacy systems
Repetitive tasks like updating records or syncing information across older systems are automated to improve accuracy and save time.
Enterprise integrations
Nintex connects with your existing systems to keep claim data, approvals, and reporting aligned, allowing teams to work efficiently without switching between tools.
Nintex User Ratings on G2
|
Evaluation Area
|
Nintex Score
|
|
G2 Aggregate Rating
|
4.3 on G2
|
|
Alignment With Business Needs
|
8.4
|
|
User Friendliness
|
8.4
|
|
Implementation Simplicity
|
8.0
|
|
Administration Experience
|
8.0
|
|
Support Experience
|
8.1
|
|
Partnership Satisfaction
|
8.4
|
|
Roadmap Confidence (% Positive)
|
8.1
|
Nintex’s user ratings on G2
Nintex’s Pros and Cons
Pros:
- Intuitive no-code interface for fast workflow and form creation.

Source
- Strong automation with good cross-system integration support.
- Adapts well to both simple and complex processes.

Source
- Quick setup without requiring heavy technical expertise.
Cons:
- Pricing becomes expensive as workflows, environments, and users scale.

Source
- Requires governance and technical oversight for complex process implementations.

Source
- Advanced customization often requires developer involvement beyond that of business users.

Source
7. ProcessMaker
Best for: Data and document-heavy claims automation
ProcessMaker’s Homepage
ProcessMaker helps teams automate data-heavy workflows and streamline document-driven processes, reducing manual effort and allowing you to focus on more strategic work. It connects your systems, extracts data from unstructured documents, and guides you in building optimized workflows using AI. Its flexible, API-first design makes it easier to integrate automation into your existing tools.
Key features of ProcessMaker
Intelligent document processing (IDP)
You can automatically extract structured data from invoices, forms, contracts, and other unstructured documents. As a result, your teams spend less time on manual data entry and process documents more quickly and more accurately.
API-first integrations
ProcessMaker connects with your existing platforms and services, so your workflows stay integrated across the systems you already use.
AI-assisted process building
AI helps you design and optimize workflows by suggesting steps and improvements, letting you create efficient processes without starting from scratch.
Visual workflow designer with role assignments
You can map out each workflow visually, assign responsibilities at every step, and ensure accountability, so tasks move smoothly through your team from start to finish.
ProcessMaker User Ratings on G2
|
Category
|
ProcessMaker Rating
|
|
Overall
|
4.3 on G2
|
|
Meets Requirements
|
8.6
|
|
Ease of Use
|
8.6
|
|
Ease of Setup
|
7.8
|
|
Ease of Admin
|
8.1
|
|
Quality of Support
|
8.2
|
|
Has Been a Good Partner in Doing Business
|
8.3
|
|
Product Direction (% positive)
|
8.2
|
ProcessMaker’s user ratings on G2
ProcessMaker’s Pros and Cons
Pros:
- Flexible platform supporting diverse workflow automation scenarios.
- Reliable and supportive customer team offering a high level of customer satisfaction.

Source
- Good customization for tailored business process automation.

Source
- Accessible automation for users with minimal coding skills.

Source
Cons
- Missing features in branding and integration capabilities.

Source
- Performance issues across browsers and complex implementations.

Source
- Extensive training is required for consistent platform access.
8. Pipefy
Best for: Visual, stage-based workflow tracking
Pipefy homepage
For teams that prefer visual stage tracking, Pipefy uses pipeline-style workflows to manage finance requests, HR approvals, and service intake. You can track tasks as they move through predefined stages, giving your team a clear view of work status at any time.
Key features of Pipefy
Shareable forms and portals
You can create forms and portals for anyone to submit requests, which are automatically routed into your workflows.
Email-to-process conversion
Emails sent to designated addresses are converted into process tickets in Pipefy, allowing your team to capture requests from email without changing how they work.
Process connections across departments
Work can automatically move between teams, providing visibility across departments and reducing delays and miscommunication.
Public API for custom integrations
Pipefy’s API lets you integrate with other systems and extend functionality when pre-built connectors aren’t available, keeping your workflows flexible and connected.
Pipefy User Ratings on G2
|
Category
|
Pipefy Rating
|
|
Overall
|
4.6 on G2
|
|
Meets Requirements
|
8.7
|
|
Ease of Use
|
9.2
|
|
Ease of Setup
|
8.9
|
|
Ease of Admin
|
8.7
|
|
Quality of Support
|
8.8
|
|
Has Been a Good Partner in Doing Business
|
8.9
|
|
Product Direction (% positive)
|
9.4
|
Pipefy’s user ratings on G2
Pipefy’s Pros and Cons
Pros:
- Very easy to use for non-technical teams building automated workflows.

Source
- Quick automation setup without needing coding or complex configurations.

Source
- Clean, user-friendly interface for organising and tracking process stages.
Source
- Improves team collaboration through structured and visual workflow management.

Source
Cons:
- Premium features can become expensive as usage and team size grow.

Source
- Limited native integrations with essential tools like Jira, Slack, and Notion.

Source
- Occasional glitches may interrupt workflow automation and process consistency.
6 Benefits of Claims Management Software
Let’s explore the top benefits of implementing claims management software:
Faster claims processing
Claims move through structured intake and approval stages with fewer manual interruptions. Automated routing replaces informal follow-ups, thereby shortening resolution timelines and reducing processing variability across teams.
Cost savings
Manual coordination, document handling, and repetitive administrative work decline as workflows become standardized. Over time, this lowers the cost per claim and improves productivity without increasing headcount.
Improved customer service and responsiveness
Clear status visibility allows insurers to communicate more accurately with claimants. Resolution timelines become more predictable, and fewer delays build stronger trust in sensitive claim situations.
Reduced claims data errors
Data validation and controlled workflow steps create consistency in how information is captured and reviewed. This minimizes discrepancies that typically arise in email-driven or spreadsheet-based processes.
Better compliance and audits
Every action within a claim is recorded automatically, creating a defensible audit trail. Regulatory reviews become less disruptive because documentation is already structured and accessible.
Enhanced analytics with centralized reporting and live dashboards
Centralized reporting provides insight into operational bottlenecks, workload distribution, and claim trends. Leadership teams gain visibility that supports continuous refinement rather than reactive problem-solving.
How to Choose Claims Management Software That Actually Works for You (In 2 Steps)
Choosing claims management software requires alignment with your operational model and long-term regulatory exposure. Here are the steps you can follow while making a selection:
Step 1. Evaluate your vendors and narrow down your options.
Use this checklist to narrow down your options when evaluating vendors:
Integration and system fit
- Connects with policy administration, billing, and CRM systems
- Eliminates duplicate data entry across platforms
Scalability
- Handles your current claims volume without performance issues
- Supports growth across new products, regions, or business lines
- Can scale without requiring a full system replacement
Compliance and security
- Meets your industry’s regulatory requirements
- Provides audit trails and activity logs
- Includes role-based access controls
- Encrypts sensitive data
Ease of use
- Simple, intuitive interface for adjusters and managers
- Reduces training time
- Simplifies task tracking and communication
Vendor support
- Clear onboarding plan
- Training included
- Responsive, reliable customer support
- Ongoing product updates and improvements
Total cost of ownership
- Transparent pricing structure
- No hidden fees for users or integrations
- Clear understanding of 3–5 year costs
Time to value
- Realistic and short implementation timeline
- Clear milestones to measure ROI
- Early operational improvements expected post go-live
Step 2. Evaluate the necessary features that matter most in modern claims software.
Next, look for the following core features in the best claims management software for your organization:
AI assistants
Modern platforms increasingly use AI to reduce manual effort. Intelligent assistants can respond to claimant inquiries in real time, summarize claim histories, surface policy details, and guide next steps. Fewer repetitive questions for your team and faster service for your customers.
Claims workflow customization
Your claims process is unique. Whether you handle insurance, healthcare, or workers’ compensation, your workflows should reflect your rules, approvals, and escalation paths.
Look for a system that lets you configure workflows without heavy development. You should be able to adapt processes as regulations or business needs change.
Intelligent claims automation
Repetitive tasks slow your team down. Registration, documentation checks, adjudication steps, and payment approvals can all be automated.
Automated routing and validation rules reduce manual errors, freeing your adjusters to focus on complex cases.
Fraud detection and risk assessment
Fraud prevention protects your bottom line. Strong systems use AI-driven analytics and predictive models to flag suspicious patterns, assess risk levels, and prioritize investigations.
Early detection reduces financial loss and protects operational efficiency.
Built-in regulatory compliance
Compliance should never feel like an afterthought. Look for the following features:
- Built-in audit trails
- Role-based access controls
- Data encryption
- Regular compliance updates
Regulations change over time, and your claims management system should adapt just as quickly. It should automatically stay aligned with evolving legal and compliance requirements, so you do not have to track and manage that risk manually.
Which Is The Best Claims Management Software?
After reviewing these eight platforms, one thing is clear: the best choice depends on what you are trying to improve in your claims operation. Here’s our honest takeaway on the best claims management software:
- If you are replacing or modernizing a full core claims system, platforms like Guidewire ClaimCenter or BriteCore make sense because they provide deep, end-to-end insurance functionality within an integrated core environment.
- For orchestrating complex, long-running claims across multiple enterprise systems, Appian offers strong case management and governance capabilities.
- If you are focused on automating structured, approval-heavy workflows without replacing your core system, FlowForma stands out for its no-code flexibility, structured routing, and faster time to value.
- Tools like Kissflow or Pipefy offer simpler, approval-driven processes, while Nintex and ProcessMaker are better suited to document-heavy or data-intensive automation scenarios.
Ultimately, the right platform is the one that aligns with your operational complexity, compliance requirements, and growth plans.
Claims management delivers the most value when you gain control over complex cases without slowing down resolution.
For insurers using Microsoft 365, FlowForma removes the friction often associated with digitizing claims workflows. Processes run where your teams already collaborate, claim data stays within your existing security and retention framework, and audit trails are captured automatically as part of daily operations.
AI Copilot reduces the time needed to design and standardize claims workflows. Instead of relying on email follow-ups and manual coordination, your team can move to structured, rule-based execution without long development cycles.
If your goal is to run compliant, approval-driven claims at scale while keeping process ownership with the business and governance with IT, FlowForma supports that operating model. Explore a live demo or start a 7-day free trial to see it in action.
.png)